|Author: Hency Kushwah|
The Promise Behind the Vaccine
HPV is a group of viruses linked to several cancers, most notably cervical cancer. Public health agencies argue that vaccination against certain high-risk strains of HPV can significantly reduce the long-term risk of developing these cancers.
Globally, the vaccine market is dominated by three major products:
These vaccines have received approval from multiple regulators and are recommended by organizations such as the World Health Organization in many national immunization programs. Supporters argue that widespread vaccination could eventually eliminate cervical cancer as a major global health threat.
However, large scale medical programs inevitably raise questions about safety, ethics, and transparency.
Side Effects and Safety Monitoring
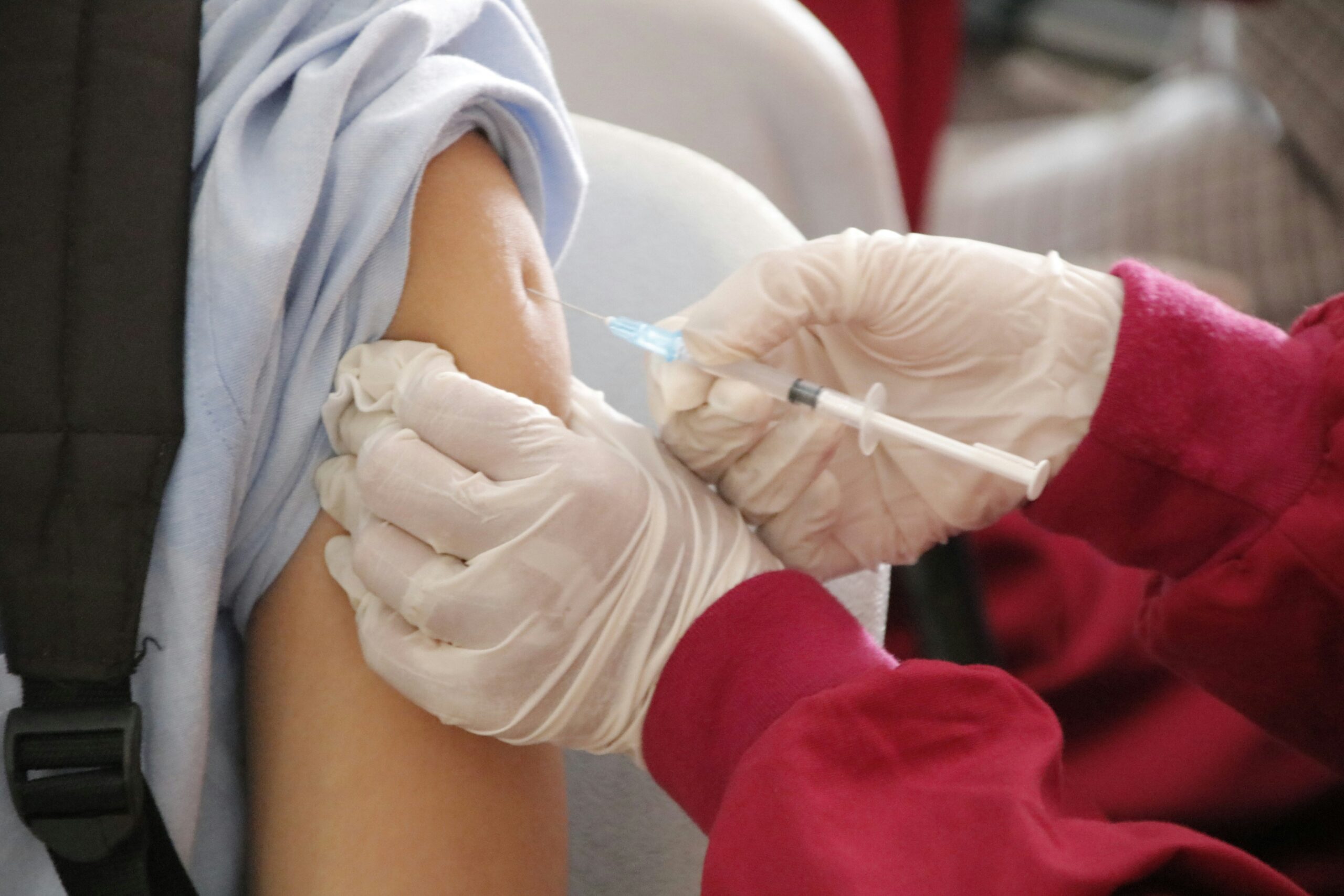
Like any pharmaceutical product, HPV vaccines carry potential side effects. Health authorities acknowledge common reactions, including pain at the injection site, fever, headaches, fatigue, and dizziness. Fainting after vaccination has also been reported, particularly among adolescents.
More controversial are reports from some individuals who have claimed more serious symptoms following vaccination, including chronic fatigue, neurological problems, and autoimmune conditions. Regulatory agencies generally state that large epidemiological studies involving millions of vaccine recipients have not established a consistent causal link between the vaccine and such conditions.
Nevertheless, critics argue that adverse event monitoring systems can be imperfect. In many countries, vaccine safety surveillance relies on passive reporting systems, meaning complications may be underreported or difficult to investigate conclusively. This gap between official safety assessments and public concerns continues to fuel debate.
India’s HPV Vaccine Controversy
India’s most significant HPV controversy emerged in 2009 during a demonstration project involving thousands of adolescent girls in Andhra Pradesh and Gujarat. The project was conducted by the global health organization PATH in collaboration with state governments and supported through international vaccine initiatives that included funding connected to the Bill & Melinda Gates Foundation.
Several deaths occurred among participants during the project period. Later investigations determined that the deaths were not directly caused by the vaccine, but the episode triggered widespread scrutiny.
In 2013, India’s Parliamentary Standing Committee on Health issued a strongly critical report on the program. The committee highlighted serious concerns, including:
The committee concluded that ethical norms governing clinical research had not been adequately followed. The controversy temporarily halted HPV vaccination programs in parts of India and continues to shape public skepticism about large-scale immunization campaigns.
In October 2025, reports from the Saharsa district in Bihar stated that 30–35 schoolgirls fainted after receiving the HPV vaccine during a school vaccination drive. The students were taken to a local hospital, and district authorities later stated that the situation was under control.
Global Health Funding and Influence
Another layer of the HPV vaccine debate concerns the growing role of philanthropic organizations in shaping global health policy. The Bill & Melinda Gates Foundation has become one of the largest private contributors to international public-health programs, funding initiatives through organizations such as the World Health Organization and Gavi, the Vaccine Alliance.
Supporters argue that such funding has accelerated vaccine access in low-income countries and strengthened global disease-prevention efforts. Critics, however, raise questions about the influence of private donors on international health priorities.
Academic debates around “philanthrocapitalism” have examined whether large private foundations may indirectly shape policy agendas in ways that national governments or public institutions alone might not have chosen.
These concerns extend beyond HPV vaccines and reflect a broader conversation about accountability and transparency in global health governance.
Acceptance and Debate Worldwide
Despite controversies, HPV vaccination programs have expanded steadily across the globe. More than 125 countries have integrated HPV vaccines into national immunization schedules.
Many medical organizations argue that the scientific evidence supporting HPV vaccination remains strong, pointing to studies showing declining rates of HPV infection and precancerous cervical lesions in vaccinated populations.
At the same time, skepticism persists in some communities, particularly where past controversies or regulatory failures have undermined public confidence. Several countries have faced public protests or calls for additional safety reviews, demonstrating that vaccine policy often intersects with politics, ethics, and public perception.
The Core Issue: Trust in Public Health
The HPV vaccine debate illustrates a broader challenge for modern medicine. Scientific research, pharmaceutical innovation, and global health initiatives operate within complex systems of regulation, funding, and public communication.
When transparency appears limited or ethical standards are questioned, public trust can weaken quickly. Conversely, when health authorities openly address concerns, provide clear data, and maintain robust safety monitoring, confidence can be rebuilt.
Ultimately, the conversation surrounding HPV vaccination is not simply about a single vaccine. It reflects the ongoing tension between scientific progress, regulatory oversight, and the public’s right to informed consent.
For individuals and policymakers alike, the central task remains the same: to examine evidence carefully, demand accountability from institutions, and ensure that public health decisions remain grounded in both science and transparency.






